Pam Fichtner,
RMT | Breast and Chest Health Educator | Founder, Sephira Healing | Saskatoon, Saskatchewan
TL;DR "Breast pain is one of the most common things I see in my practice — and it's almost never what you're afraid it is."
- Most breast pain is not cancer — up to 70% of women experience it at some point
- The most common causes are hormonal changes, fibrocystic tissue, lymphatic congestion, and muscle tension
- Cyclical pain that follows your menstrual cycle is very common and usually not a concern
- Gentle movement, deep breathing, and lymphatic drainage massage therapy can help ease many types of breast discomfort
- See a doctor if you notice a new lump, skin changes, nipple discharge, or pain that doesn't improve or feels unusual for your body
Could this be breast cancer?
Breast pain (mastalgia) can be scary and we almost immediately fear that any pain there could be a sign of cancer. But breast pain alone is rarely a symptom of breast cancer. In fact, the majority of breast discomfort is caused by hormones, muscle tension, or lymphatic congestion — all very manageable and very common.
I'm Pam Fichtner, a Registered Massage Therapist, breast and chest health educator, and a court-recognized expert witness in breast massage therapy for Saskatchewan. I founded Sephira Healing in Saskatoon in 2004, and over 30 years of clinical experience, I've had the privilege of supporting women, trans, and nonbinary people across Canada, including many navigating surgery, recovery, and life with or beyond cancer.
Studies suggest that up to 70% of women will experience breast pain at some point in their lives, which is very much in line with what I see in my practice.
Breasts are living tissue. They respond to hormones, stress, posture, movement, and even how we breathe.
So, the key to understanding your breast health is noticing changes in your own body. When you become familiar with how your breasts normally feel, it becomes much easier to notice when something changes.
Before we look at some of the common causes of breast pain, remember that articles like this are meant to provide education, not a diagnosis.
If something in your breast or chest area feels different from what is normal for you, trust that instinct and speak with your healthcare provider.
Hormonal Changes: What Does Hormonal Breast Pain Feel Like?
Hormonal fluctuation is one of the most common causes of breast pain, and it usually shows up as tenderness or swelling 1–2 weeks before your period. That’s often when estrogen and progesterone can cause breast tissue to hold more fluid.
This type of breast pain is cyclical, meaning it tends to follow the same pattern each month and usually improves once menstruation begins and hormone levels shift again.
You might feel:
- Heaviness
- Soreness
- Swelling
- sensitivity to touch
Some people I treat at Sephira Healing also notice that the discomfort spreads into the armpit or upper chest area, which can feel alarming but is also common with hormonal breast pain.
Hormonal breast pain can also happen during:
- perimenopause
- pregnancy
- hormone therapy
- certain birth control methods
During these transitions, the body is adjusting to new hormone levels, and the breast tissue may respond differently than it has in the past.
For many people, this type of discomfort settles as hormone levels stabilize. However, if breast pain feels unusual for your body, persists beyond your normal cycle, or is concentrated in one specific area, it’s always a good idea to speak with your healthcare provider.

Fibrocystic Breast Tissue: Is Lumpy or Tender Breast Tissue Normal?
Yes, in most cases it is. Up to 50% of women between the ages of 20 and 50 experience fibrocystic breast changes at some point in their lives. It’s a very common and non-cancerous condition.
Fibrocystic breast changes happen when fibrous tissue thickens or small fluid-filled cysts develop within the breast.
Breast tissue is not meant to feel perfectly smooth. It's naturally dense, with areas that may feel lumpy or rope-like. Because breast tissue responds to hormones, these changes often become more noticeable before menstruation, when estrogen and progesterone cause the breast tissue to swell and hold more fluid.
People with fibrocystic breast tissue may notice:
- areas that feel lumpy or rope-like
- tenderness or sensitivity
- swelling or fullness
- breast discomfort that changes during the menstrual cycle
These sensations can feel concerning, especially if you’re not familiar with how your breast tissue normally feels. But in many cases, the discomfort improves once menstruation begins and hormone levels shift again.
When you know what is normal for your body, it becomes much easier to notice when something truly changes.
At Sephira Healing, I often encourage clients to do a breast self-exam at the same time each month, ideally a few days after their period when breast tissue is not as sensitive or tender.
If you ever feel a new lump does not move, continues to grow, or even just feels different from the rest of your breast tissue, it’s always a good idea to speak with your healthcare provider.
Lymphatic Congestion: Can Slow Lymph Flow Cause Breast Tenderness?
Yes. And it's more common than most people realize! The breasts are part of the lymphatic system, which helps move fluid, waste, and immune cells throughout the body. Unlike your heart, the lymphatic system has no pump, so it relies entirely on movement, breath, and muscle activity to keep fluid circulating.
That’s why lymph fluid can sometimes move more slowly, especially when we’re sitting a lot, holding tension in our chest and shoulders, or not moving as much as usual.
When that lymph flow slows, some women experience:
- fullness
- tenderness
- swelling
- heaviness in the chest
Gentle movement, breath, and massage therapy can really help and support that healthy lymphatic flow.
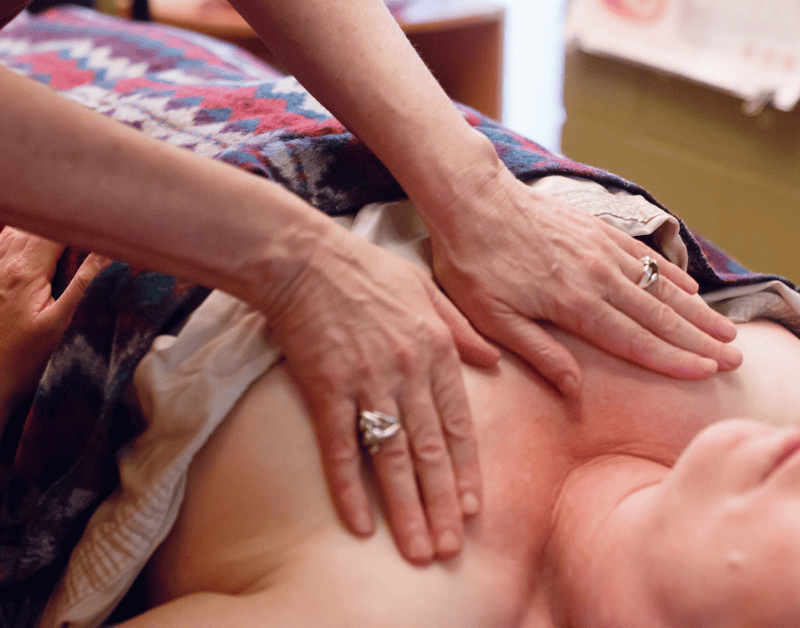
Lymphatic drainage massage is something many of my clients at Sephira Healing now ask for specifically. It’s a very gentle technique that encourages lymph fluid to move through the body and toward nearby lymph nodes, where it can be filtered and returned to circulation. This can help improve lymph circulation, reduce swelling, and ease discomfort after surgery, injury, or lymphedema.
Because the lymphatic system relies on movement to function well, I also help my clients with some gentle stretching, breathing, and yoga poses that support healthy lymph flow. These four are the ones I recommend most often for the upper body:

4 Yoga Poses to Support Lymphatic Flow in the Chest
- Seated neck stretch — helps encourage lymph movement through the neck, shoulders, and upper chest. Sit upright and gently lower your head toward your chest or shoulder, holding the stretch for about 30 seconds.
- Supine reclined twist — helps stimulate circulation through the torso and chest. Lie on your back and gently bring one knee across your body into a soft twist while keeping your shoulders relaxed.
- Child's pose — gently stretches the back, shoulders, and chest while encouraging slow, deep breathing. From hands and knees, sit your hips back toward your heels and rest your torso forward.
- Cat–cow pose — helps mobilize the spine and rib cage while supporting breath and movement through the chest. Alternate slowly between arching and rounding your back.
For the full list of 8 poses with detailed instructions, [see this post.]
These movements don’t need to be intense. Slow, gentle motion and steady breathing are usually enough to help support your body’s natural lymphatic flow.
Stress and Muscle Tension: Can Stress and Tight Muscles Cause Breast Pain?
Yes. Breast pain doesn’t always come from breast tissue. Muscles in the chest, ribs, and shoulders can also refer pain into the breast area.
Even when the breast tissue itself is healthy, stress and poor posture can create tension in the muscles of the chest, shoulders, and rib cage, which may make the breasts feel sore or sensitive.
When these muscles become tight, they can create pressure and pulling sensations through the chest wall, which may be felt as soreness, tenderness, or sensitivity in the breasts.
Many people spend long hours sitting at desks, leaning forward, or looking down at phones. This position can tighten the chest muscles while weakening the muscles in the upper back, creating imbalance and tension through the chest and rib cage.
When we are stressed, breathing often becomes short and shallow, which limits movement in the rib cage and chest. Over time this can contribute to tightness and discomfort in the surrounding muscles and connective tissue.
This tension can show up in a few different ways, including:
- tight chest muscles
- shallow breathing
- shoulder tension
- fascial restriction
In many cases, gentle movement, stretching, massage therapy, and mindful breathing can help release this tension and allow the chest to relax again.
However, if breast pain persists, worsens, or feels different from what is normal for your body, it’s important to speak with your healthcare provider to rule out other causes.

Improper Support: Can a Poor-Fitting Bra Cause Breast Pain?
Yes. And it is one of the most overlooked causes of breast and chest discomfort.
Wearing a poorly fitting or unsupportive bra can place ongoing strain on the muscles, ligaments (often called Cooper’s ligaments), and connective tissue of the chest, shoulders, and upper back. Over time, that strain can show up as tenderness, achiness, or a general heaviness in the breast and chest area.
This is especially common during exercise, when breast tissue needs adequate support to reduce excessive movement, and for people with larger breasts, where the weight of unsupported tissue can place constant pull on the chest wall and surrounding muscles.
At Sephira Healing, bra fit is something I bring up regularly with clients. Here’s a few questions that can help you determine if it’s your bra that’s contributing to discomfort:
- Does your bra feel tight across the chest band or dig into your shoulders?
- Are you relying on the straps for most of the support rather than the band?
- Does your bra fit differently at different times of the month as your breast tissue changes?
If breast and chest discomfort seems to worsen during activity or by the end of the day, I’d recommend visiting a professional bra fitter to ensure your bra is providing the right support for your body.
7 Simple Daily Habits That Can Help Ease Breast Discomfort
Because the breasts are influenced by hormones, circulation, muscle tension, and lymphatic flow, small daily habits can sometimes make a big difference in how your chest feels. At Sephira Healing, these are the ones I recommend most often.
- Gentle movement throughout the day – walking, stretching, or light yoga helps support circulation and lymphatic flow.
- Taking breaks from sitting – standing up, rolling the shoulders, or stretching the chest can relieve tension that builds in the rib cage and shoulders.
- Slow, deeper breathing – diaphragmatic breathing helps the rib cage expand and contract, which naturally supports lymph movement.
- Rebounding or light bouncing – gentle bouncing on a mini trampoline can help stimulate lymphatic circulation because the lymphatic system responds well to rhythmic movement and changes in gravity.
- Supporting lymphatic flow with massage therapy – gentle self-massage or professional lymphatic drainage massage therapy can help encourage fluid movement through the lymphatic system.
- Staying hydrated – I remind my clients that the lymphatic system is largely fluid, and drinking enough water throughout the day is one of the simplest things you can do to support it.
- Wear a well-fitting, supportive bra - Breast size and shape changes over time. So, make sure you’re routinely fitted for the correct bra size.
When Should Breast Pain Be Checked by a Doctor?
As I often remind my clients, the most important part of breast health is knowing what is normal for your own body. When you become familiar with how your breasts normally feel, it becomes much easier to recognize when something changes.
Most of the time, breast pain is related to hormones, muscle tension, lymphatic flow, or other non-serious causes. But if you notice a change that feels unusual for you, it’s always a good idea to speak with a healthcare provider.
Here are 6 clear signs of breast pain or changes you should get checked by your healthcare provider:
- a new lump that feels different from the surrounding tissue
- a lump that does not move or continues to grow
- skin dimpling, puckering, or changes in the texture of the skin
- nipple discharge that is new or unusual
- redness, warmth, or swelling in the breast
- pain that persists or does not improve over time
If you’re experiencing breast or chest discomfort and would like support understanding what your body might be telling you, you don’t have to navigate that alone.

You Don't Have to Navigate This Alone
Even though breast and chest pain is common, and in most cases has a straightforward explanation, I also know that "common" doesn't make it any less scary when it's happening in your own body.
My goal at Sephira Healing is to help you feel more at ease in your body and more confident in what it's telling you.
If you're curious about breast and chest health, or looking for evidence-based support that feels comfortable and safe, I invite you to book a session or sign up for a class.
Many clients tell me they didn't know how much they needed this kind of support until they experienced it. For a lot of people, it's the first time they've ever stopped avoiding this part of their body. You don't have to wait for pain or a crisis to happen before you start caring for your whole body.
[Explore Classes] [Book a Session]
FAQ’S:
Frequently Asked Questions About Breast Pain
Is breast pain a sign of cancer?
In most cases, no. Breast pain is actually one of the less common symptoms of breast cancer. Most breast pain is related to hormonal changes, fibrocystic breast tissue, lymphatic congestion, or muscle tension — all very common and manageable causes. That said, if you notice pain accompanied by a new lump, skin changes, nipple discharge, or anything that feels unusual for your body, it's always worth speaking with your healthcare provider. Knowing your own body is the most important tool you have.
Why do my breasts hurt before my period?
This is one of the most common questions I hear at Sephira Healing, and the answer is usually hormones. In the 1–2 weeks before your period, estrogen and progesterone levels rise and cause breast tissue to swell and hold more fluid. This can create tenderness, heaviness, and sensitivity that typically improves once your period begins and hormone levels shift again. If the discomfort feels more intense than usual or is concentrated in one specific area, it's a good idea to check in with your healthcare provider.
Is it normal to feel lumps in my breast tissue?
Yes — breast tissue is not meant to feel perfectly smooth. It's naturally dense, and many people have areas that feel lumpy, rope-like, or uneven. Up to 50% of women between the ages of 20 and 50 experience fibrocystic breast changes, which can make the tissue feel more pronounced at certain times of the month. What matters most is knowing what is normal for your own body so that you can notice when something truly changes. If you feel a new lump that doesn't move, continues to grow, or feels different from the surrounding tissue, speak with your healthcare provider.
Can massage therapy help with breast pain?
For many people, yes. Breast and chest massage therapy can help support lymphatic flow, ease muscle tension in the chest wall, and reduce the heaviness or fullness that comes with hormonal fluid retention. It can also help people reconnect with a part of their body they may have been avoiding. At Sephira Healing, breast and chest massage therapy is offered as evidence-based therapeutic care — not a trend, and not a cure-all. Our goal is to support your body in doing what it's already designed to do.
What is lymphatic drainage massage therapy and how does it help?
Lymphatic drainage massage therapy is a very gentle, specialized technique that encourages lymph fluid to move through the body toward the lymph nodes, where it can be filtered and returned to circulation. Unlike regular massage therapy, it uses light, rhythmic strokes specifically designed to stimulate the lymphatic vessels just beneath the skin. It can help reduce swelling, ease breast and chest tenderness, support post-surgical recovery, and improve overall circulation through the chest. I have been certified with the Dr. Vodder School for nearly 30 years and it is one of the most requested services at Sephira Healing.
Can stress really cause breast pain?
Yes — and this surprises a lot of people. Breast and chest pain doesn't always originate in the breast tissue itself. When we are stressed, breathing becomes shallow, the chest tightens, and muscles in the rib cage and shoulders can refer pain directly into the breast and chest area. Poor posture from long hours at a desk or looking down at a phone adds to this tension over time. Gentle movement, deeper breathing, and massage therapy can all help release that tension and ease the discomfort it creates.
Can a poorly fitting bra cause breast pain?
Yes — and it's more common than people realize. A bra that doesn't fit well can place ongoing strain on the muscles, ligaments, and connective tissue of the chest, shoulders, and upper back. This shows up as tenderness, achiness, or heaviness that often worsens during activity or by the end of the day. It's especially common for people with larger breasts, where unsupported tissue places constant pull on the chest wall. If you notice your discomfort increases during exercise or correlates with how long you've been wearing your bra, fit may be a contributing factor. I recommend visiting a professional bra fitter — it's a simple step that can make a surprisingly big difference. At Sephira Healing, bra fit is something I bring up regularly because the right support is genuinely part of breast and chest health care.
When should I see a doctor about breast pain?
Most breast and chest pain doesn't require urgent medical attention, but there are specific signs that mean it's time to see your healthcare provider. Reach out if you notice a new lump that feels different from the surrounding tissue, a lump that doesn't move or continues to grow, skin dimpling or puckering, nipple discharge that is new or unusual, redness, warmth, or swelling in the breast or chest, or pain that persists and doesn't improve over time. Trust your instincts. If something feels different from what is normal for you, that's reason enough to get it checked.
What can I do at home to ease breast discomfort?
Quite a bit, actually. Start with your bra. It's one of the most overlooked contributors to breast and chest discomfort, and getting properly fitted can make a surprising difference. From there, gentle movement throughout the day, slow diaphragmatic breathing, staying hydrated, and taking regular breaks from sitting can all make a meaningful difference. Gentle self-massage to support lymphatic flow is something I teach many of my clients at Sephira Healing — you don't always have to come in to get relief. Light bouncing on a mini trampoline, yoga poses that open the chest and upper body, and reducing prolonged shoulder tension are all simple, accessible tools. The more you understand what your body is responding to, the more confident you feel managing it.
What does a session at Sephira Healing involve?
Every session at Sephira Healing begins with a conversation. I want to understand what you're experiencing, what feels concerning, and what you're hoping to get from your care. Consent is explicit, ongoing, and never assumed. From there, sessions may include breast and chest massage therapy, lymphatic drainage massage therapy, craniosacral therapy, or trauma-aware somatic bodywork depending on what your body needs. Many clients also leave with simple self-care practices they can use at home. My goal is never to create dependence — it's to help you feel more informed, more comfortable, and more at ease in your own body. If you're not sure whether a session is right for you, you're welcome to reach out before booking.
Pam Fichtner, RMT | Breast and Chest Health Educator | Founder, Sephira Healing | Saskatoon, Saskatchewan
Medical References